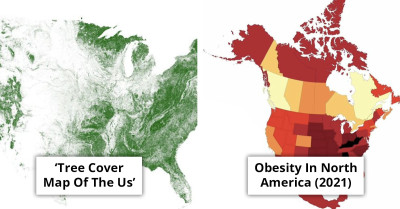
Could IBS Be Linked to 'Gravity Intolerance'? A Gastroenterologist’s Surprising Theory
Brennan Spiegel from Cedars-Sinai Medical Center in Los Angeles outlined a new hypothesis.
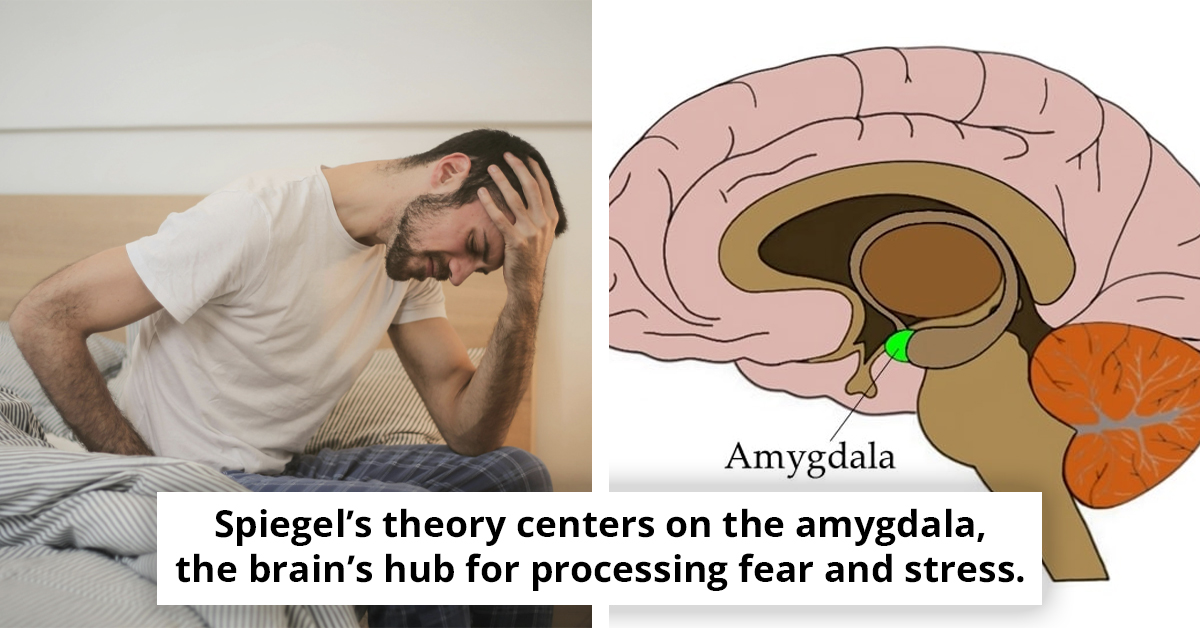
A 28-year-old woman refused to sit on the edge of her couch, not because she was clumsy, but because her stomach would start acting like the floor was about to drop out from under her. When her IBS flares, the timing feels oddly consistent, like her body is bracing for a fall that never comes.
In this surprising theory, the culprit is the amygdala, the brain’s fear-and-stress hub. The idea is that some people’s amygdala may overreact to gut signals, treating normal digestion like it’s danger, the way your body prepares you when you’re near a cliff. Now add the gut-brain axis, the well-known stress and anxiety overlap, and the fact that gravity intolerance has not been tested in controlled trials, and the whole thing gets messy fast.
It started as a “maybe it’s the fear circuit” story, but it leaves you wondering what her gut thinks gravity is doing.
The Brain-Gut Connection
At the heart of Spiegel’s theory is the amygdala, a part of the brain that plays a central role in processing fear and stress. He proposes that people with IBS may have an overreactive amygdala that misinterprets signals from the gut as signs of imminent danger.
This would make evolutionary sense. In situations where a fall or injury is likely, such as standing near the edge of a cliff, the body’s stress response could help protect us. But if the amygdala becomes overly sensitive, it might start triggering gut distress even when there is no actual threat.
Research has shown that amygdala hyperactivity is indeed more common among people with IBS, supporting at least part of Spiegel’s reasoning.
That couch-edge habit makes the amygdala explanation feel less like sci-fi and more like a pattern you can’t unsee.
The intricate relationship between the gut and the brain, commonly known as the 'gut-brain axis,' sheds light on the complexities of irritable bowel syndrome (IBS). This connection is particularly relevant in understanding why IBS is frequently linked to psychological conditions such as stress and anxiety. The article highlights a revealing study which indicates that patients suffering from IBS often report higher levels of anxiety, suggesting that the psychological state of individuals may play a crucial role in the manifestation of their digestive symptoms. This reinforces the notion that treating IBS may require a holistic approach that considers both physical and mental health aspects.
At the heart of Spiegel’s theory is the amygdala, a part of the brain that plays a central role in processing fear and stress.
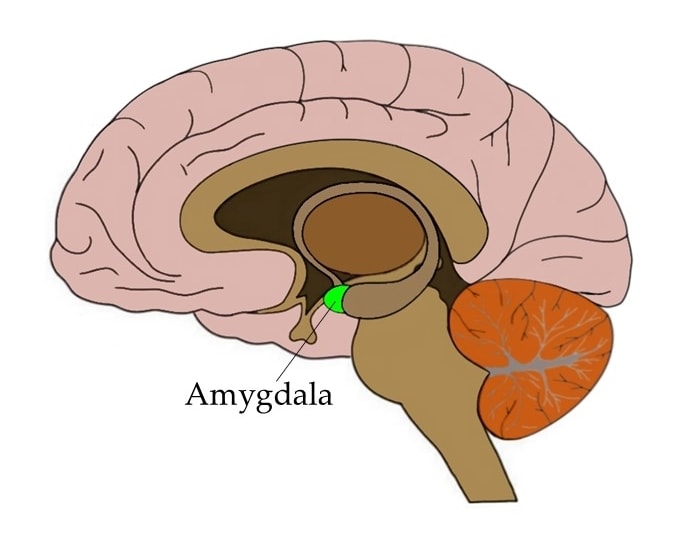 Neuroscientifically Challenged
Neuroscientifically ChallengedThe gut-brain axis section lands right after the cliff-edge logic, and suddenly stress stops sounding like a side character.
The Skepticism
Despite the intriguing nature of the idea, many scientists are quick to point out that this is just a theory. No controlled experiments or clinical trials have been conducted to test whether gravity intolerance actually plays a role in IBS.
One major flaw is that if difficulty managing gravity were a key factor, IBS rates might be higher in populations living at sea level, where gravitational force is marginally weaker compared to high elevations. But this is not the case. Iceland, for example, has high IBS rates despite its higher altitude and relatively low population density.
Despite the intriguing nature of the idea, many scientists are quick to point out that this is just a theory.
 Pexels
Pexels
Then the skepticism hits, because nobody has run the controlled gravity intolerance tests, even as IBS rates keep showing up anyway.
A New Lens for an Old Problem
Even with these criticisms, Spiegel sees value in his idea. He describes it as “a new way of thinking about old ideas” and hopes it will encourage fresh approaches to understanding and treating IBS. He refers to the concept as a “thought experiment” rather than a proven explanation, emphasizing that it is meant to open new lines of research rather than replace existing theories.
For patients, IBS often means navigating a frustrating maze of possible causes, from stress and diet to bacterial imbalances and nerve hypersensitivity. If anything, Spiegel’s hypothesis highlights how complex the gut-brain relationship truly is—and how many factors, even fundamental forces like gravity, could influence our digestive health.
While the “gravity intolerance” theory may never be fully proven, it serves as a reminder that sometimes thinking far outside the box is what moves science forward. As researchers continue to unravel the mysteries of IBS, even ideas that sound unusual at first might help lead to better treatments and a deeper understanding of how the human body works.
The “sea level” argument sticks, since you would expect different gravity exposure to change the odds if this theory were the whole story.
The concept of gravity intolerance, while not extensively explored in psychological research, echoes the experiences of those suffering from balance disorders and vertigo. These conditions not only create physical discomfort but are also often intertwined with psychological stress. The relationship between stress and physical health is well-documented, suggesting that emotional factors could play a significant role in exacerbating symptoms of gravity intolerance. This connection offers a compelling lens through which to examine the emerging theory linking IBS to gravity intolerance. As IBS symptoms can be influenced by stress and anxiety, understanding this relationship could pave the way for innovative approaches to managing this pervasive digestive disorder.
In light of the ongoing exploration into the causes of irritable bowel syndrome (IBS), it is evident that psychological factors significantly influence this disorder. The connection between stress, anxiety, and IBS is well-documented, suggesting that emotional well-being is intertwined with digestive health. The emerging theory of 'gravity intolerance' adds a compelling layer to our understanding of IBS, potentially offering a new avenue for research and treatment. It emphasizes the need for a holistic approach to managing IBS, where psychological therapies are not just supplementary but integral to treatment. Cognitive-behavioral therapy has proven to be particularly beneficial, as it empowers patients to make choices that positively affect their health in response to emotional triggers. This dual focus on both the mind and body could lead to more effective management strategies for those suffering from IBS.
Her gut might be reacting to imaginary danger, but the gravity part still has a lot of unanswered questions.
That’s a lot like the “AITA for taking stray kittens to shelter” fight with the partner who said no.