Mother, 45, initiates legal proceedings after enduring six years of chemotherapy she claims was unnecessary.
A mother’s six-year ordeal with unnecessary chemotherapy sparks legal action against the NHS, igniting a fierce debate over patient care and treatment protocols.
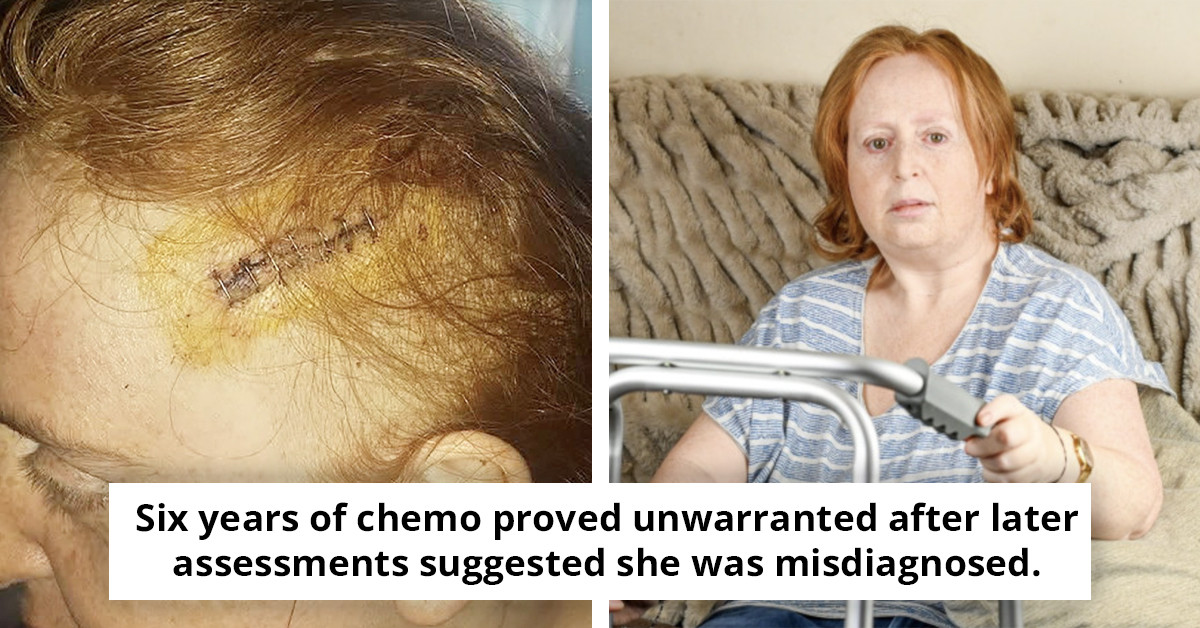
A mother from Bromsgrove, Samantha Smith, is fighting back after six years of chemotherapy she says never should have been on the menu. Now she’s wading into legal proceedings while others who went through similar NHS journeys rally behind her, pushing for answers and a deeper look at how cancer diagnoses are confirmed.
The scary part is not just the treatment, it’s the possibility that it was avoidable.

Mother Advocates for Change After Misdiagnosis in Cancer Treatment
Samantha, a mother from Bromsgrove, Worcestershire, has shared her story in hopes of sparking change within the healthcare system. After enduring a grueling six years of chemotherapy, she discovered that the aggressive treatment was not warranted, as later assessments suggested her condition may have been misdiagnosed.
This unsettling revelation has not only left her questioning the reliability of her initial care but has also led to an outpouring of support from others who have faced similar experiences with the NHS. As her legal battle unfolds, advocates are rallying for a comprehensive review of diagnostic practices to prevent future patients from enduring unnecessary treatments.
The troubling case of Samantha Smith serves as a stark reminder of the pressing need for enhanced diagnostic accuracy within the National Health Service. After enduring six years of chemotherapy that she now claims was unnecessary, the implications of potential misdiagnoses are profound. Such errors not only subject patients to undue physical and emotional suffering but also raise critical questions about the protocols that govern treatment decisions.
To prevent similar situations in the future, a more collaborative approach is essential. By encouraging multidisciplinary teams to reassess complex cases, healthcare providers could significantly reduce the risk of misdiagnosis. This strategy not only aims to minimize errors but also seeks to improve overall patient outcomes, ensuring that individuals receive the most suitable and effective treatments for their specific conditions.
Samantha Smith’s six-year chemo timeline at University Hospital Coventry is the kind of detail that makes the whole case feel even more unsettling.
Long-Term Cancer Treatment Journey at University Hospital Coventry
This diagnosis led to a series of treatments, including surgery, radiotherapy, and a prolonged chemotherapy regimen at the University Hospital Coventry. Samantha embarked on a chemotherapy journey that lasted six and a half years, a duration far exceeding standard treatment protocols.
The gravity of her situation became apparent when, during a routine MRI scan in 2021, Samantha was informed that she could potentially stop her chemotherapy treatments. However, when a new consultant took over her case, the shocking truth emerged: she had been subjected to an excessive treatment plan that was not aligned with established medical guidelines.
Consultant Reveals Chemotherapy Duration Misjudgment
The new consultant revealed that the typical duration for chemotherapy in such cases should have been limited to only six months, not the six years that Samantha had endured. She expressed her devastation, stating, “Undergoing chemotherapy is a gruelling process, and I’ve been very unwell for the best part of a decade.
But I told myself it was all worth it to get better. So to find out that around six-and-a-half years of my treatment wasn’t needed came as a huge shock.
Stolen Time: A Mother's Struggle with Health Challenges
I feel like that part of my life has been stolen from me, as I spent so long unable to function properly and just getting by day-to-day.” The emotional and physical toll of her treatment has been profound. Samantha, a mother of three, has faced numerous health challenges as a result of the chemotherapy.
She has had to take extra precautions during the COVID-19 pandemic due to her compromised immune system, which left her vulnerable to infections. The long-term side effects of the chemotherapy have severely impacted her quality of life, leading to fatigue, ongoing infections, and mobility issues.

Once her later assessments suggested the original diagnosis might be wrong, the story stopped being only about one patient and started sounding like a system-wide warning.
Struggles with Mobility Prompt Legal Action for Samantha
She described her struggles, stating that she cannot lift her right leg or move her shoulder, which has significantly hindered her daily activities. In light of her experience, Samantha has engaged legal representation to investigate her case further.
She is concerned that her situation may not be unique and that other patients may have also been subjected to unnecessary treatments.
And if you thought hospitals were strict, the cruise line’s “strict” dress code sparked backlash from guests.
See how a cruise line’s new strict dress code policy turned into a fight with travelers.
UHCW Initiates Review of Samantha's Chemotherapy Treatment
The University Hospitals Coventry and Warwickshire NHS Trust (UHCW) has acknowledged the gravity of Samantha's case and is conducting an internal review to understand the circumstances surrounding her prolonged chemotherapy treatment. In a letter to Samantha, the Trust confirmed that her treatment plan lacked scientific support and that measures have been implemented to prevent similar occurrences in the future.
This internal review is part of a broader effort to ensure that all patients receive appropriate and evidence-based care.
Devastation from Unnecessary Medication: Samantha's Struggle
She stated, “Samantha had every faith in what she was being advised, so to be told that more than six years of medication administered to her was completely unnecessary has left her devastated and with so many questions. She’s been forced to live with the side effects of the toxic drug, which have taken a significant toll on her health and quality of life.
While nothing can change what she’s been through, we’re determined to help her obtain the answers and access to specialist rehabilitation and support she deserves.” The implications of this case extend beyond Samantha's individual experience. It raises critical questions about the protocols and decision-making processes within the NHS, particularly regarding the treatment of complex conditions such as high-grade brain tumors.
As Samantha’s legal battle unfolds, the support pouring in from others who’ve faced similar NHS treatment decisions turns her experience into a larger fight.
Challenges and Prognosis of High-Grade Brain Tumors
High-grade brain tumors, such as glioblastomas, are notoriously difficult to treat and are associated with poor prognoses.
The complexity of treating such conditions necessitates a careful balance between aggressive treatment and the potential for adverse effects. The National Institute for Health and Care Excellence (NICE) provides guidelines that allow clinicians to exercise professional judgment when determining treatment plans.

The case of Samantha Smith highlights a critical need for a reevaluation of treatment protocols within the UK's National Health Service. After enduring six years of chemotherapy, which she asserts was unnecessary for her brain tumor, Smith's experience raises significant concerns about the adherence to evidence-based medicine in patient care.
Unnecessary treatments, such as prolonged chemotherapy, can inflict severe physical, emotional, and financial tolls on patients. This situation underscores the urgent necessity for healthcare systems to conduct regular reviews of treatment guidelines. Such measures could prevent similar distressing cases in the future, reaffirming that patient safety and well-being must be at the forefront of medical practice.
Ensuring Oversight in Adjuvant Temozolomide Treatment
However, the case of Samantha Smith highlights the potential for misjudgment and the need for rigorous oversight in treatment protocols. The UHCW Trust has commissioned the Royal College of Physicians to conduct an independent review of patients who received more than twelve cycles of adjuvant temozolomide (TMZ) treatment between 2017 and 2023.
This review aims to ensure that all patients receive appropriate care and to identify any systemic issues that may have contributed to Samantha's over-treatment. As this investigation unfolds, it is crucial for healthcare providers to reflect on the importance of evidence-based practice and the need for continuous education and training for medical professionals.
That’s where the pressure ramps up for a review of diagnostic practices, because nobody wants another family to watch years of treatment unfold on shaky ground.
Prioritizing Patient Safety: Lessons from Medical Errors
The emotional and physical consequences of medical errors can be devastating for patients and their families, and it is essential that healthcare systems prioritize patient safety and quality of care. In conclusion, Samantha Smith's case serves as a poignant reminder of the complexities and challenges faced by patients undergoing treatment for serious medical conditions.
The emotional turmoil and physical toll of unnecessary treatments can have lasting effects on individuals and their families. As the investigation into her case continues, it is imperative that the NHS takes the necessary steps to ensure that such incidents do not occur in the future.
Empowering Patients Through Safe and Transparent Healthcare Practices
The commitment to providing safe and effective care must remain at the forefront of healthcare practices, and patients must be empowered to seek answers and advocate for their health and well-being. The broader implications of this case highlight the importance of transparency and accountability within the healthcare system.
Patients deserve to have confidence in their treatment plans and to trust that their healthcare providers are acting in their best interests. As the NHS navigates this challenging situation, it is essential for all stakeholders to work together to improve patient care and outcomes, ensuring that no one else has to endure the unnecessary suffering that Samantha has experienced.
Justice Through Advocacy: A Case of Medical Negligence
This case not only underscores the need for rigorous adherence to clinical guidelines but also emphasizes the importance of patient advocacy and the role of legal recourse in addressing medical negligence. As Samantha seeks justice for the years lost to unnecessary treatment, her story may inspire others to speak out and seek accountability within the healthcare system.
Ultimately, the goal must be to create a healthcare environment where patients receive the best possible care based on the latest scientific evidence, where their voices are heard, and where their well-being is the top priority. The lessons learned from Samantha's experience can serve as a catalyst for change, fostering a culture of safety and excellence in patient care across the NHS and beyond.
The situation faced by Samantha Smith highlights a pressing demand for transparency and accountability within the NHS. Her claim of undergoing six years of unnecessary chemotherapy raises serious concerns about the adequacy of current diagnostic methods and treatment protocols. The lack of regular reviews in these areas can lead to significant patient distress and suffering.
To address these issues, it is essential for the NHS to foster collaborative practices among healthcare professionals and prioritize patient-centered care. By implementing these changes, the NHS can improve the quality of its services and ensure that patients like Smith receive treatments that are both effective and appropriate, ultimately leading to better health outcomes for all.
Samantha Smith is basically asking the NHS to explain how six and a half years of chemo could happen in the first place.
Want another surprising health wake-up call? Read how a dog’s alertness led a woman to breast cancer care.
For another family showdown, check out what a 36-year-old woman says her dog did before her life-saving breast cancer diagnosis.